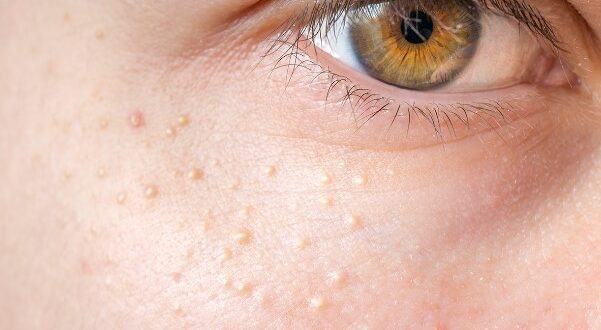
Milialar, more commonly known as milia, manifest as small, dome-shaped bumps that are typically white or yellowish. They occur when keratin, a protein that’s a key component of skin, hair, and nails, becomes trapped beneath the surface of the skin, forming cysts. These benign formations are widespread and can affect individuals across various age groups, from infants to adults. Despite their harmless nature, many people seek treatment due to cosmetic concerns, especially since they often appear on the face, usually around the nose and cheeks.
The development of milia is not tied to poor hygiene or any specific lifestyle factors but is rather a natural occurrence that can happen to anyone. The primary type usually forms on areas rich in sebaceous glands and may resolve spontaneously without intervention. Secondary milia, however, can develop after trauma or damage to the skin such as burns, blisters, or as a result of certain skin conditions.
Understanding the nature of milialar is advantageous for managing and preventing these skin occurrences. Recognizing the distinct characteristics of milia, which include their appearance, typical locations, and the conditions under which they form, can aid in early identification. Although milia are mostly painless and do not cause acute symptoms, those seeking removal options can consult with dermatologists for appropriate treatments that ensure the preservation of skin health and aesthetics.
Understanding Milialar
Milialar, as a term, is multifaceted and its relevance varies across different contexts. With its roots in diverse origins, it generally symbolizes the interplay of various factors or concepts. However, when discussing milia in dermatological terms, understanding milialar requires comprehension of the skin’s keratinization process—one aspect of skin cell biology.
Milia are small, cyst-like bumps that appear on the skin’s surface. They form when keratin, a protein found in skin cells, becomes trapped beneath the surface of the skin. Keratin is an essential component that protects the skin against damage and stress, but when overproduced or not exfoliated, it can lead to these tiny, pearl-like cysts.
The formation of milia is not limited by age and can affect both infants and adults. Common areas for the appearance of these cysts include around the eyes, cheeks, and forehead. Though they are usually harmless, their presence can be a cosmetic concern for individuals:
| Feature | Description |
|---|---|
| Appearance | Whitish-yellow, small, dome-shaped pearly bumps. |
| Common Locations | Around the eyes, cheeks, forehead, and eyelids. |
| Size | Typically 1-2 millimeters in diameter. |
Genetic factors may play a role in an individual’s predisposition to milia, although research is ongoing. The understanding of genetics in relation to skin conditions like milia remains complex, with many contributing elements under investigation.
When it comes to treating milia, the focus is often on gentle exfoliation and, if necessary, professional procedures. They commonly resolve on their own, especially in infants, but it’s essential to consult a dermatologist if they persist, especially to avoid self-removal attempts that can lead to skin damage.
Causes of Milialar

Milialar, commonly known as milia, occurs due to various factors ranging from genetic predisposition to environmental triggers. These factors influence the formation of tiny, keratin-filled cysts primarily on the skin.
Genetic Factors
Some individuals are genetically predisposed to developing milia. This inherent tendency means that milia can occur as a part of natural skin characteristic for certain people, even without specific external triggers.
Skin Cell Accumulation
Primary milia are often a result of dead skin cells accumulating in sweat ducts or on the skin surface. In newborns, it’s due to immature sweat glands, while in adults, it may be due to cells not exfoliating naturally.
Skin Trauma and Damage
Secondary milia can develop following skin damage, such as:
- Burns: Heat damage can lead to blistering and milia upon healing
- Trauma: Skin injuries can cause cysts where the skin repairs itself
Beauty and Skincare Products
Heavy creams and skincare products that are not non-comedogenic can clog pores, leading to the formation of milia. Products should allow skin to breathe and cells to exfoliate naturally to prevent milia.
Environmental Factors
Excessive sun exposure toughens the skin and impedes normal shedding, which can contribute to milia. Using sun protection can help prevent the sun damage that leads to the development of these skin cysts.
Medications and Health Conditions
Certain medications and medical conditions can cause milia as a side effect. This includes drugs that affect skin cell turnover or conditions that cause blistering. It’s essential to consider underlying health issues when addressing the causes of milia.
Types and Symptoms of Milialar
Milialar manifests through distinctive types and symptoms, each with particular characteristics. Understanding these aspects is vital for recognition and differentiation of the condition.
Primary Milia
Primary milia occur spontaneously and are common among infants but can also affect adults. They are typically formed when keratin, a protein in the skin, becomes trapped beneath the skin surface. The cysts are usually found on areas such as the face, especially around the eyes, cheeks, nose, and forehead.
- Complexion impact: Little to no effect; milia are not usually associated with discoloration
- Size: Approximately 1-2 millimeters in diameter
- Color: White or yellowish
- Texture: Firm, dome-shaped bumps
Secondary Milia
Secondary milia result from an injury or trauma to the skin that leads to clogged sweat ducts. It’s also associated with a history of certain skin conditions or the use of heavy creams that obstruct skin pores. In contrast to primary milia, secondary milia can result upon healing from the condition that caused them.
- Common causes: Skin conditions, trauma, and use of occlusive skincare products
- Potential sites: Anywhere on the body where trauma or skin healing is taking place
Location and Appearance
Milia can be pinpointed to specific facial areas and exhibit a characteristic appearance that aids in their identification.
- Common locations: Face (eyes, eyelids, cheeks, nose, forehead).
- Appearance: Small, round, and raised.
| Appearance Characteristic | Detail |
|---|---|
| Size | Typically 1-2 millimeters |
| Color | Whitish-yellow |
| Shape | Dome-shaped |
| Texture | Smooth, pearly cysts on the skin |
Common Symptoms
Despite being generally painless, the presence of milia can sometimes be accompanied by other sensations or secondary symptoms.
- Painless: Milia generally don’t cause pain
- Itching or Discomfort: Rare, but possible if surrounding skin is irritated
Note: Symptoms vary between individuals and may not necessarily indicate an underlying skin condition, especially in newborns where milia are common and typically resolve without intervention.
Diagnosis and Professional Care

When suspecting the presence of milialar, it is essential for individuals to seek professional healthcare guidance for accurate diagnosis and advice on appropriate treatment options.
Clinical Assessment
A dermatologist’s clinical assessment is the first step in diagnosing milialar. During the examination, they will inspect the affected skin areas to identify the characteristic small white bumps that define milialar. They will take note of their distribution, size, and the presence of any associated features that might suggest underlying skin conditions. Healthcare professionals may discuss the patient’s skin care routine, as improper practices can sometimes contribute to the formation of milia.
Diagnostic Procedures
If the clinical assessment does not conclusively diagnose milialar, or if there is suspicion of another underlying condition, the dermatologist may perform additional diagnostic procedures. A biopsy can be conducted to rule out other possibilities and confirm the diagnosis. This procedure involves taking a small sample of skin tissue from the area displaying milia for detailed laboratory analysis. Treatments are then tailored based on the accurate diagnosis, considering patient-specific factors to ensure the most effective results.
Treatment Options for Milialar
For individuals seeking to manage milialar, commonly known as milk spots, a variety of treatment options exist that focus on both removal and prevention of these small cysts.
Medication and Topical Treatments
For mild cases of milialar, topical treatments such as retinoids and keratolytic agents like salicylic acid or glycolic acid can be effective. These compounds facilitate the shedding of the outer layer of skin, preventing the formation of new milia and aiding in the removal of existing ones.
- Topical Retinoids: Encourages cell turnover, potentially reducing milia over time
- Salicylic Acid: Helps to unclog pores by exfoliating the skin surface
- Glycolic Acid: Another exfoliant, it helps in refreshing the skin’s appearance
Manual Extraction and Procedures
Manual extraction, performed by a professional dermatologist or aesthetician, involves sterilized tools such as a needle to create an opening in the skin, allowing the content of milia to be carefully extracted.
- Cryotherapy: Freezes the milia, making them easier to remove
- Laser Therapy: A targeted approach that uses light to diminish milia
Chemical and Physical Exfoliations
Stronger treatments include chemical peels and microdermabrasion. These procedures aid in exfoliation and may require a series of sessions for optimal results.
- Chemical Peels: Acidic solutions are applied to the skin to peel away layers and reduce milia
- Microdermabrasion: Uses fine crystals or a diamond-tip wand to exfoliate and reduce the appearance of milia
Preventive Skincare
An effective skincare routine can prevent the recurrence of milialar. This includes using non-comedogenic products to avoid clogged pores and incorporating gentle exfoliation into a regular skincare practice.
- Non-comedogenic Products: Less likely to clog pores, these are vital for milia-prone skin
- Gentle Exfoliation: Regular, non-abrasive exfoliation can prevent dead skin cell accumulation
Prevention Strategies

Effective prevention of milialar, commonly known as milia, involves a multi-faceted approach that focuses on skin care, sun protection, and overall health. Implementing key strategies can significantly reduce the incidence of these small, white skin bumps, especially with consistent care.
Sun Exposure Management
Sunscreen Application: Regular use of sunscreen is imperative to protect the skin from excessive sun exposure, which can exacerbate milialar. It is recommended to apply a broad-spectrum sunscreen with at least SPF 30 to all exposed areas daily, even during cloudy days.
- Sunglasses and Hats: Alongside sunscreen, wear sunglasses and wide-brimmed hats for added sun protection, particularly during the hours of peak UV radiation
Skincare and Cosmetic Recommendations
Gentle Cleansing and Exfoliation: Incorporate a gentle cleansing routine to keep the skin clear of excess oils and debris. Gentle exfoliation can aid in the removal of dead skin cells, but should be done sparingly to prevent irritation.
- Non-Comedogenic Products: Choose skincare and cosmetic products labeled non-comedogenic to avoid clogging pores, which is a known cause of milialar
Healthy Lifestyle and Habits
Balanced Diet: A healthy diet rich in vitamins and minerals supports skin health and can aid in the prevention of milialar. Adequate hydration is also crucial for maintaining skin elasticity and minimizing the effects of aging.
- Avoid Heavy Creams: Steer clear of using heavy creams, especially on areas prone to milia. Instead, opt for lightweight, hydrating formulas that are less likely to cause blockages
Ongoing Monitoring and Care
Regular Dermatologist Visits: Schedule regular check-ups with a dermatologist to monitor skin changes and receive personalized advice on preventing milialar. They can provide tailored recommendations based on your skin type and history.
- Adapt Skincare Routine: Be open to adjusting your skincare routine as needed, taking into account any skin changes due to aging or environmental factors, to maintain its effectiveness in milialar prevention
Additional Information
In this section, readers will find a curated selection of content offering deeper insight into milialar, with topics ranging from common inquiries to potential natural treatments and cosmetic impacts.
Frequently Asked Questions
What are milialar, often referred to as milk spots?
Milialar, or milk spots, are tiny cysts filled with keratin that typically appear on the skin as small, white bumps. They are particularly common in newborns, a condition known as neonatal milia, and are usually found on the nose, cheeks, and chin.
Can milialar affect a person’s complexion?
Yes, milialar can be a cosmetic concern for some, impacting the smoothness and uniformity of the complexion. However, they are generally benign and often resolve without treatment.
Natural Remedies and Alternatives
Tea Tree Oil: Known for its antibacterial properties, tea tree oil may be used cautiously to address the underlying skin issues leading to milialar. However, one should never apply it undiluted to the skin.
Honey: As a natural humectant and anti-inflammatory, honey can be applied to the skin to help maintain moisture and reduce inflammation.
Cosmetic Considerations
Is extraction an option for milialar?
Professional extraction can be performed by a dermatologist but is typically reserved for persistent cases that do not resolve on their own.
Can over-the-counter products help with milialar?
Products containing salicylic acid or alpha hydroxy acids may help to gently exfoliate the skin and promote the turnover of dead skin cells, potentially reducing the appearance of milialar. It’s important to use such products as directed to avoid irritation.